We have access to some of the best equipment for imaging the retina and help diagnosing retinal conditions.
Macular Degeneration
The commonest retinal conditions we treat are macular degeneration, retinal vascular occlusions and diabetic retinopathy.
There are several options like laser and injections available for treatment and we would be happy to discuss these with you at the time of your consultation.
Age-related macular degeneration (AMD) is an eye disease that causes vision loss in the centre of vision. It is caused by the deterioration of the macula which is located at the back of the eye. AMD is the leading cause of legal blindness for people over age 50. AMD is present in approximately 10% of the population over age 52 and in up to 33% of individuals older than 75.
Types of AMD
There are two types of macular degeneration: Dry AMD and Wet AMD.
Dry AMD occurs when small clumps of protein and fat called drusen form under the macula. This condition can also occur when the basement layer under the retina degenerates.
Wet AMD occurs when new blood vessels grow under the macula, leaking blood and fluid that cause the macula to blister.
Dry AMD in may develop Wet AMD over time.
Symptoms of AMD
Dry AMD symptoms usually develop gradually. Vision loss is typically severe and rapid with Wet AMD, Symptoms can include:
Blurry or hazy vision
Difficulty seeing in dim light
Difficulty recognizing faces
Blind spot in central vision
Dullness of colours
Straight lines appear wavy
Because AMD does not cause pain or irritation, the symptoms can easily be overlooked.
CAUSES AND TREATMENT OF AMD
There is no singular cause of AMD.
Some risk factors may include:
Age
Genetics / family history of AMD
Smoking
Female gender
Light-coloured eyes
Fair coloured skin
Poor nutrition
High cholesterol
Cardiovascular disease
Treatment of AMD
There is no cure for AMD; however, there are treatments that can slow the progression of the disease. It is also important to stop smoking as this is one of the biggest risk factors for developing macular degeneration.
Dry AMD Treatment: A good healthy diet of fruit, green vegetables, and oily fish is helpful in slowing down progression of dry AMD. There are preparations with combinations of vitamins with high doses of antioxidants and zinc available over the counter, but these are only really useful for those whose diet is deficient.
Wet AMD Treatment: Injections of anti-angiogenic medications into the eye can prevent development of new blood vessels and reduce leakage from existing blood vessels.

Amsler Chart
The Amsler grid eye test is used to help macular degeneration patients manage their condition and alert them to any changes in their condition. This is a simple test that can be done at home.
1. Tape this page at eye level where light is consistent and without glare.
2. Put on your reading glasses and cover one eye.
3. Fix your gaze on the center black dot.
4. Keeping your glaze fixed, try to see if any lines are distorted or missing.
5. Mark the defect on the chart.
6. Test each eye seperately
7. If the distortion is new or has worsened, arrange to see your eye doctor at once.
8. Always keep the Amsler's chart the same distance from your eyes the each time you test.
DIABETIC EYE CARE
The retina (nerves at the back of the eye) needs a continual supply of blood and nutrients to stay healthy. If the blood vessels that supply blood to the retina begin to deteriorate and leak fluid and blood into the retinal tissue, the health of the retina is put in jeopardy.
The condition of diabetic retinopathy is a complication of diabetes. It is estimated that over 25% of diabetics have some form of this disease. It is the leading cause of blindness in adults with diabetes.
Symptoms of Diabetic Retinopathy
In the early stages, a patient with diabetic retinopathy may not know that damage is occurring because there are no outward symptoms. This increases the importance for diabetics to have regular eye exams that will identify these silent diseases; treatment can then be started that can slow progression of the disease.
In the later stages, diabetic retinopathy can cause:
Vision loss
Blindness
Blurry vision
Dark spots, strings or floaters in the vision
Colour perception difficulties
Retinal detachment
Glaucoma
Vitreous haemorrhage (the jelly-like substance that fills the eye)
Causes of Diabetic Retinopathy
Elevated blood sugar levels can damage or even completely block the blood vessels that nourish the retina. This can occur in either Type I or Type II diabetics. Other risk factors for diabetic retinopathy include high blood pressure, high cholesterol, tobacco usage and pregnancy.
Treatment for Diabetic Retinopathy
Lifestyle changes to control blood sugar levels will dramatically reduce the risk of developing diabetic retinopathy. It can also help to slow the progression of the disease.
If you have been diagnosed with the disease, treatment will depend on the severity of your condition. Treatment may include:
Injections into the eye to reduce the retinal swelling or stop new blood vessels from growing.
Vitrectomy to remove blood from the vitreous area of the eye
Laser treatment to slow or halt the leakage of fluid in the eye or to shrink abnormal blood vessels
RETINAL VEIN OCCLUSIONS
A retinal vein occlusion occurs when one of the veins in the retina is blocked and cannot drain blood from the retina. This blockage causes damage to the vein and leads to a backup of blood, leading to leaking of blood and fluid which can be seen as haemorrhages and swelling (oedema) of the retina.
The block can be in a smaller (branch) or major (central) retinal vein.
Risk factors associated with retinal vein occlusions include high blood pressure, glaucoma, blood clotting disorders, and age. All patients with retinal vein occlusions should be evaluated by their GP to ensure blood pressure and other risk factors are adequately controlled.
Symptoms
Blurred vision
Distortion (straight lines appear wonky)
New floaters (floating black spots in vision)
Pain due to raised eye pressure
Some patients do not have any symptoms
Treatment
The blockage cannot be reversed. The swelling can be treated with injections to the eye. We use the drug aflibercept which has been shown to have better results in such conditions (LEAVO Trial).
Laser retinal treatment can also be an option in certain patients.
OTHER MACULAR DISEASES
The macula is a small collection of nerve cells found in the middle of the retina (the back of the eye). Responsible for our central vision, this is the sharp point where the eye focuses the images that we see. When a break develops in these nerve fibers, this is called a macular hole. As we age, the macula can also begin to grow a thin layer of scar tissue over the light-sensitive surface. This is a macular pucker.
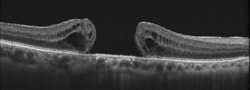
Macular Holes
Symptoms of Macular Holes
Macular holes are painless but they can seriously affect your vision as you grow older. Most people develop these after age 60; women are more susceptible to the disease.
Symptoms can include:
Loss of central vision
Distortion/blurriness of central vision
Straight lines that look wavy
Left untreated, the symptoms will continue to worsen.
Macular Pucker
Symptoms of Macular Pucker (epiretinal membrane)
A macular pucker can have some of the same symptoms as a macular hole, although this is not the same as a macular hole and severe vision loss is uncommon with this condition.
Symptoms can include:
Blurry central vision
Mildly distorted central vision
Straight lines look wavy
Difficulty reading small print
Gray spot in central vision
Blind spot in central vision
Causes of Macular Holes
Macular holes can be caused by:
Diabetic eye disease
Macular pucker
Detached retina
Eye trauma or injury
Shrinkage or detachment of the vitreous (jelly-like substance) in the eye
Extreme myopia (nearsightedness)
Treatment of Macular Holes
Macular holes are most often treated surgically with a procedure known as a vitrectomy. During a vitrectomy surgery, the vitreous gel in the middle of the eye is removed and replaced with an air/gas bubble. The bubble pulls the edges of the hole together and keeps it together as the hole heals.
The bubble dissipates on its own and the eye replaces it with its own saline fluid. We are successful in achieving anatomic success in about 85-90% of cases. This, however does not always translate into improved vision. The natural lens is also usually removed a the same time, especially in those over 60 years old.
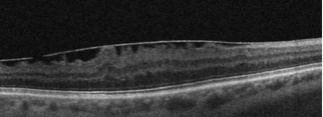
Causes of Macular Pucker
Macular pucker is often caused by the shrinkage or detachment of the vitreous (jelly-like substance) in the eye. When the vitreous pulls away from the retinal surface (a very normal occurrence) the retina will begin to heal the damaged area and form scar tissue. When this occurs on other areas of the retina, there is usually no effect on central vision; however, if it forms on the macula and begins to wrinkle, central vision will be affected. Eye trauma and prior eye surgery can also have an impact on the vitreous and lead to a macular pucker.
Treatments for Macular Pucker
Most macular pucker patients do not require any type of treatment if the symptoms are mild. However, if the distortion is affecting daily activities, a vitrectomy surgery may be performed to remove the vitreous gel to prevent it from pulling on the retina, replacing it with a saline solution. The scar tissue is also removed. This surgery is effective in restoring clearer central vision after a few months.

If you have any concerns regarding any of these conditions, then please get in touch with us.
For more information please don't hesitate to call us on 07468 204541 or fill in the form below and one of our advisors will be in contact with you shortly



